The global health landscape is continually reshaped by evolving disease patterns, and few conditions exemplify this more starkly than Parkinson's disease. A neurodegenerative disorder characterized by motor symptoms like tremor, rigidity, and bradykinesia, alongside a spectrum of non-motor manifestations, Parkinson's is increasingly recognized as a burgeoning worldwide health crisis. Recent epidemiological insights, including a compelling "bathtub analogy," illuminate the complex dynamics driving the observed surge in its global prevalence. This analogy provides a powerful framework for understanding how the inflow of new cases, the outflow of mortality, and the lack of curative treatments combine to create a steadily rising reservoir of individuals living with this debilitating condition across continents. As populations age and environmental factors continue to be scrutinized, comprehending these underlying principles becomes paramount for effective public health planning and resource allocation on a global scale.
The Bathtub Analogy: Demystifying Disease Dynamics
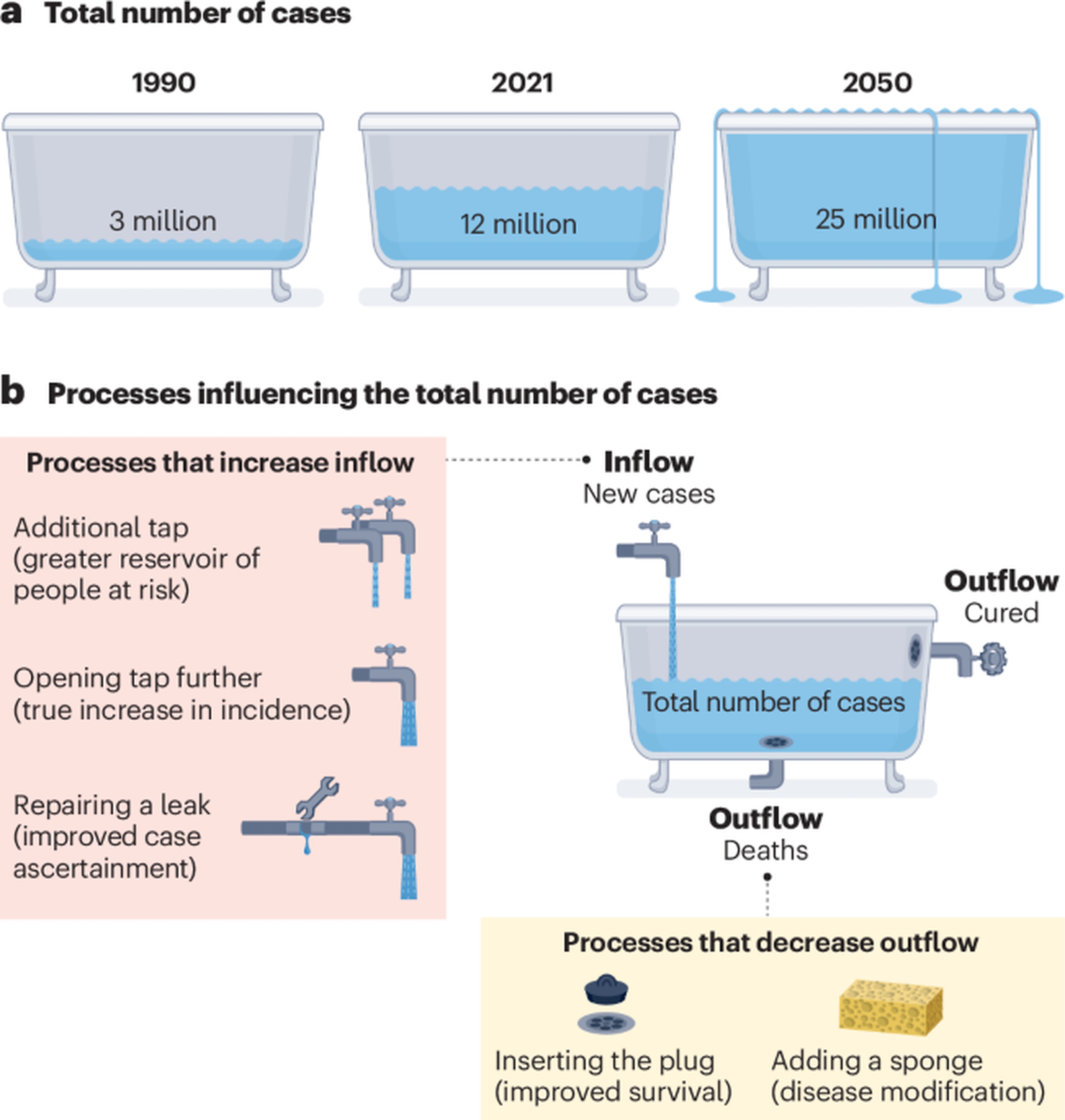
At the heart of understanding the global growth of Parkinson's disease lies a simple yet profound epidemiological model: the bathtub analogy. Imagine a bathtub where the "water level" represents the total number of people living with Parkinson's disease at any given time – its prevalence. This water level is influenced by two primary forces: the faucet, which pours in new cases (incidence), and the drain, which removes individuals from the living patient pool (mortality or, hypothetically, a cure). The current global situation suggests a bathtub where the faucet is running steadily, and the drain is either partially clogged or simply too small to cope with the influx, leading to an ever-increasing volume of water.
Inflow: The Stream of New Diagnoses
The "faucet" in our analogy, representing the incidence of Parkinson's disease, is influenced by several critical factors. A primary driver is the global demographic shift towards an aging population. Age is the single greatest risk factor for Parkinson's; as more people live longer, a larger proportion will inevitably reach the age where the disease is more likely to manifest. This demographic reality alone accounts for a significant portion of the rising incidence. Beyond age, ongoing research points to a complex interplay of genetic predispositions and environmental exposures. While genetics play a role in a minority of cases, environmental toxins, such as certain pesticides and industrial chemicals, are increasingly implicated as potential triggers, though definitive causal links remain challenging to establish. Improved diagnostic capabilities also contribute to the "inflow" of identified cases. As medical professionals become more adept at recognizing early symptoms and diagnostic tools become more refined, individuals who might previously have gone undiagnosed or misdiagnosed are now accurately identified, adding to the reported incidence. This doesn't necessarily mean more people are getting the disease, but rather that more people are being counted.
Outflow: Mortality and the Absence of Cure
The "drain" of the bathtub analogy represents the factors that remove individuals from the living patient pool. Historically, Parkinson's disease was associated with a shortened life expectancy. While it is not directly a fatal disease, its complications, such as falls, aspiration pneumonia, and other infections, can significantly increase mortality rates. However, advancements in symptomatic treatments, supportive care, and management of complications have, paradoxically, led to people with Parkinson's living longer lives. This improved longevity means that individuals, once diagnosed, remain in the "bathtub" for an extended period. Crucially, unlike many other diseases, there is currently no cure for Parkinson's disease. Once diagnosed, the condition is progressive and lifelong. The absence of a drain that completely empties the tub – a cure – means that the water level will continue to rise as long as the faucet is running, even if the flow rate remains constant. This combination of improved survival and the lack of a cure significantly contributes to the escalating prevalence.
The Rising Water Level: Understanding Prevalence
The "water level" in the bathtub, representing the prevalence of Parkinson's disease, is the net result of these inflow and outflow dynamics. When the rate at which new cases are diagnosed (incidence) outpaces the rate at which individuals exit the patient pool (mortality, or a hypothetical cure), prevalence inevitably rises. The global data unequivocally shows this upward trend. Projections indicate that the number of people living with Parkinson's disease is set to double in many regions over the coming decades. This increase is not merely a statistical anomaly but a reflection of profound demographic shifts, environmental considerations, and the current limitations of medical science in halting or reversing the disease's progression. Understanding this interplay is vital for policymakers and healthcare systems grappling with the immense burden posed by this neurodegenerative condition.
Demographic Shifts and Environmental Pressures
The relentless march of global aging is arguably the most significant demographic factor contributing to the rise in Parkinson's prevalence. As life expectancy increases across developed and developing nations alike, the proportion of the population entering the age bracket most susceptible to Parkinson's disease grows substantially. This demographic wave creates an inherent increase in the pool of at-risk individuals. Concurrently, environmental factors continue to be a subject of intense scrutiny. Exposure to certain pesticides, heavy metals, and industrial solvents has been linked to an elevated risk of Parkinson's in various studies. While the precise mechanisms are still being unravelled, the widespread presence of these agents in the environment, particularly in agricultural and industrial regions, raises concerns about their cumulative impact on global incidence rates. The interaction between genetic predispositions and these environmental triggers is also a critical area of ongoing research, suggesting a complex etiology rather than a single causative agent.
The Diagnostic Lens: Sharper Vision, Higher Numbers
Beyond the actual increase in incidence, improved diagnostic capabilities and heightened awareness among both the public and medical community play a substantial role in the observed rise in Parkinson's prevalence. Decades ago, Parkinson's disease was often diagnosed in its later stages, or even misdiagnosed, leading to an underestimation of its true burden. Today, with greater understanding of its early motor and non-motor symptoms, and the development of more sophisticated diagnostic criteria and imaging techniques (though definitive biomarkers are still sought), clinicians are better equipped to identify the disease earlier and more accurately. This enhanced diagnostic acumen means that more individuals are being correctly identified and entered into the "bathtub" of diagnosed cases, contributing to the perceived increase in prevalence, even if the underlying biological incidence rate has not changed proportionally. Public health campaigns and patient advocacy groups have also raised awareness, encouraging individuals to seek medical attention for subtle symptoms, further contributing to earlier and more frequent diagnoses.
The Socioeconomic Ripple Effect
The escalating global prevalence of Parkinson's disease carries profound socioeconomic implications. Healthcare systems worldwide are facing an unprecedented challenge in providing long-term care, medication, and supportive therapies for a growing number of patients. The chronic, progressive nature of the disease necessitates continuous medical management, rehabilitation services, and often, significant caregiver support. This places immense financial strain on individuals, families, and national healthcare budgets. Beyond direct medical costs, there are indirect costs associated with lost productivity, premature retirement, and the emotional toll on caregivers. The need for specialized neurological care, access to medications (which can be expensive), and community support services becomes more acute with each passing year, demanding innovative and sustainable solutions from governments and international organizations. Addressing this challenge requires not only medical advancements but also robust social support structures and equitable access to care.
Charting a Course Forward: Research and Global Collaboration
In the face of this global health challenge, intensive research and international collaboration are more critical than ever. Efforts are underway to identify reliable biomarkers for early diagnosis, develop neuroprotective therapies that can slow or halt disease progression, and ultimately, discover a cure. Understanding the complex interplay of genetic and environmental factors is crucial for developing preventative strategies. Global research consortia are pooling data and expertise to accelerate discoveries, recognizing that no single nation can tackle this multifaceted problem alone. Furthermore, public health initiatives aimed at reducing exposure to identified environmental risk factors, coupled with enhanced screening programs for at-risk populations, could play a vital role in mitigating future incidence. The "bathtub analogy" underscores the urgency: to control the rising water level, we must either slow the faucet (reduce incidence) or open the drain (find a cure or more effective treatments that prolong healthy life without increasing the burden of severe disease).
Conclusion: A Unified Global Response
The worldwide growth of Parkinson's disease, effectively illustrated by the epidemiological "bathtub analogy," represents a formidable and escalating global health crisis. It is a complex phenomenon driven by the inexorable forces of an aging global population, potential environmental exposures, and the current absence of disease-modifying or curative treatments. As the number of individuals living with Parkinson's continues to climb, the imperative for a unified global response becomes ever clearer. This response must encompass accelerated scientific research, robust public health strategies focused on prevention and early detection, equitable access to comprehensive care, and sustained support for patients and their families. Only through concerted international efforts can humanity hope to stem the tide of this debilitating neurodegenerative disease and improve the quality of life for millions affected worldwide.
Support Nivaran Foundation's global health initiatives to advance research and care for neurodegenerative diseases worldwide.
Support this work